
Smart Claims
Powered by award-winning AiDA technology, Amplify Health’s new and improved Smart Claims solution offers a suite of AI-enabled products designed to empower health insurers with enhanced claims processing and medical cost management.
500k
Hospital invoices digitised for straight-through claims
$3m+
Claims savings captured (USD) per 100,000 pre/post-hospitalisation claims processed
65m
Claim lines processed through our clinical encoder across 4 Asia markets
In just 2 years, Smart Claims has empowered many insurers across 7 Southeast Asia markets with enhanced claims processing capabilities and greater medical cost control.
55%
Of all MediShield claims in Singapore
Hong Kong
Thailand
Vietnam
Malaysia
Singapore
Philippines
Indonesia
Pre-Authorisation
A comprehensive pre-approval process adjudicated by AI
- Increased STP rates to over 70% through automated handling of simple cases.
- Effective cost control of treatment expenses
- Improved Net Promoter Scores (NPS) due to quicker claims disbursement, with 60% of all minor claims settled within one business day
- Policy holders receive confirmation of coverage amounts before the procedure(s) take place

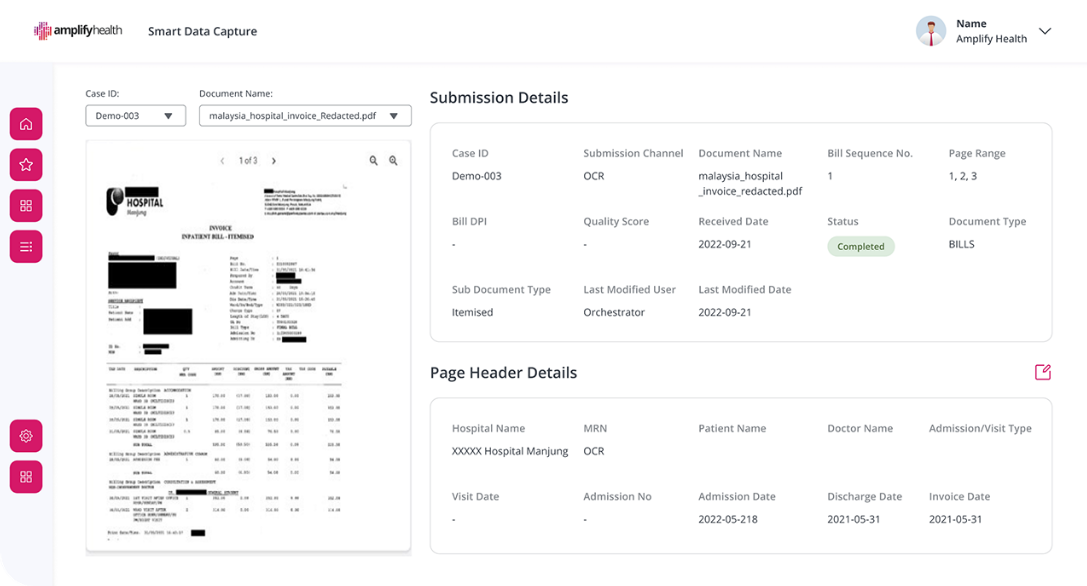
Smart Data Capture
Leverage the latest OCR tech and NLP Large Language Models
By applying business logic, post processing techniques and verification algorithm to the OCR process, extracted text is digitally converted into organised datasets with high precision, reducing fallouts and rework.
The solution is designed for Humans-in-the-Loop (HITL), who provide secondary validation on the OCR/NLP outputs and ensure clean data is transmitted downstream.
Multiple-page processing
Our engine can combine multiple pages into a single bill and return the bill level result.
Post-processing work
Inclusive of classification, header and line level extractions, and result validations.
Validations and business requirement settings
Bespoke setup according to your own controls and standards.
Clinical Encoder
Uses AI powered software to automatically map free text to standardized coding for creation of clinically rich data.
Automate Claims Adjudication: Clinical Encoder facilitates the application of complex clinical rules and policy exclusions, enabling faster, more accurate auto-adjudication of claims.
Enhanced FWA Detection: Dive deeper into provider billing practices and identify wasteful expenditures at an individual item level.
Risk and Opportunity Detection: Identify key drivers of claims experience through meaningful claim groupings, allowing for proactive risk mitigation and opportunity identification.
Clinical Encoder Features
Suite of pre-trained coding pipelines support for multiple languages ensures global applicability
“Human-in-loop” pipelines drive clinically robust, auditable processes, with expert clinical coders to compliment an existing team.
Strong governance framework ensures auditable processes and compliance with AI and data governance regulations
Flexible deployment options (batch or API) cater to diverse use cases
Comprehensive suite of clinical schemas - allows for identification of different types of FWA
AI-Driven Decision Engine
Real-time, data-driven recommendations for assessors to make faster decisions.
Utilisation of past claims data and learning algorithms. Train the decision-making model and predict decisions - Accept, decline or partial pay.
Forecasting and recommendation of claims decisions. Based on semantic connections between ICD codes and policy exclusions.
Decline without explanation. These recommendations are provided at both the claims and policy level.
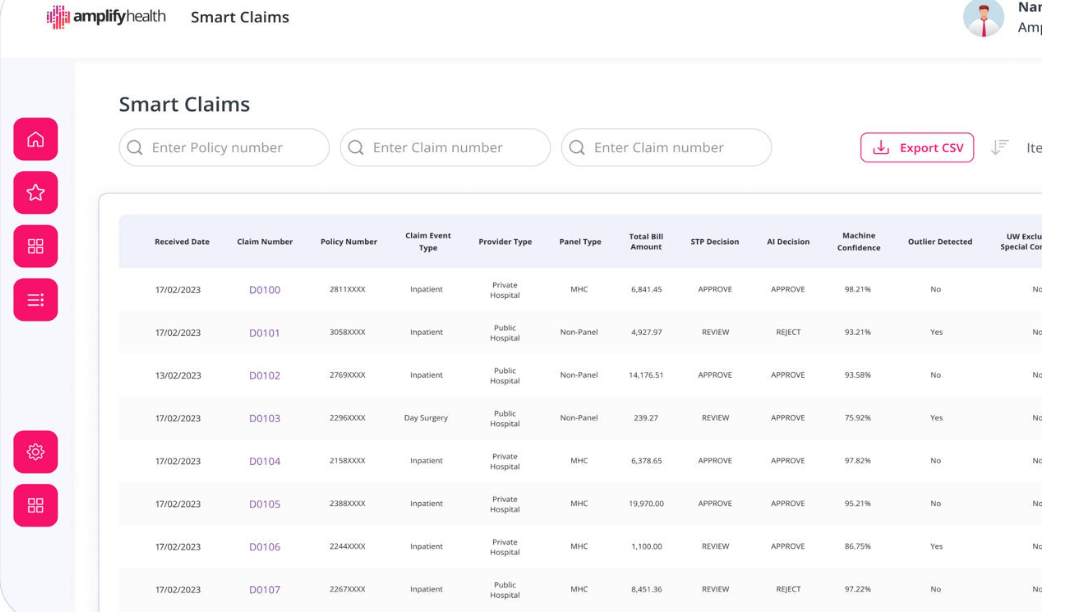
Decision Engine Benefits
Higher STP rates driven by AI-enabled decision-making, providing an increase in operational efficiency
Digitisation of paper claims
Detection of Fraud Waste and Abuse to control medical leakage and mitigate financial risks
Fraud, Waste
& Abuse Detector
Identify suspicious behavours and collusive practices in your network
A state-of-the-art ensemble of sophisticated multi-dimensional modules aimed at detecting FWA. It reduces medical leakage through the detection of:
- Claims outliers
- Suspicious provider and member behaviours
- Collusion practices
- Rules adherence (rules-based sensors)
Our detection algorithms include:
Rule-Based Sensor
Harnesses the publicly available Clinical Decision Support Rules and internal SOPs.
Outlier Detection
Catches unusually high values that do not fit into a comparable peer set.
Behaviour Sensor
Identifies changes in an entity’s behaviour pattern over a time period.
Collusion Detection
Spot inappropriate or collusive practices across your network.

Ready to enhance claims processing and reach a new level of medical cost management?

All representations of outcomes and key results referenced herein are based on previous engagements. Actual product-specific results may vary depending on eligibility criteria for claims processing, pre-existing solutions, and current assessor practices, where applicable. For Clinical Encoder, the actual results may vary based on data quality and variability.